Overview
Blue Cross Blue Shield (BCBS) generally provides coverage for Ozempic for individuals diagnosed with Type 2 diabetes. However, it is important to note that coverage may vary depending on specific insurance plans and the documentation of medical necessity. Patients are required to submit evidence of their diabetes diagnosis, along with records of prior treatment attempts. Understanding the coverage criteria is essential, as it can significantly enhance the chances of obtaining approval for the medication.
Introduction
Navigating the complexities of health insurance can often feel overwhelming, particularly when securing coverage for essential medications like Ozempic. This GLP-1 receptor agonist is recognized for its effectiveness in managing Type 2 diabetes and facilitating weight loss. A critical question arises for many: does Blue Cross Blue Shield provide coverage for this treatment? Understanding the nuances of insurance policies, including eligibility requirements and potential hurdles, is essential for patients seeking this medication. What steps can individuals take to ensure they receive the necessary benefits, and how can they effectively address challenges that may arise during the approval process?
Understand Ozempic: What It Is and How It Works
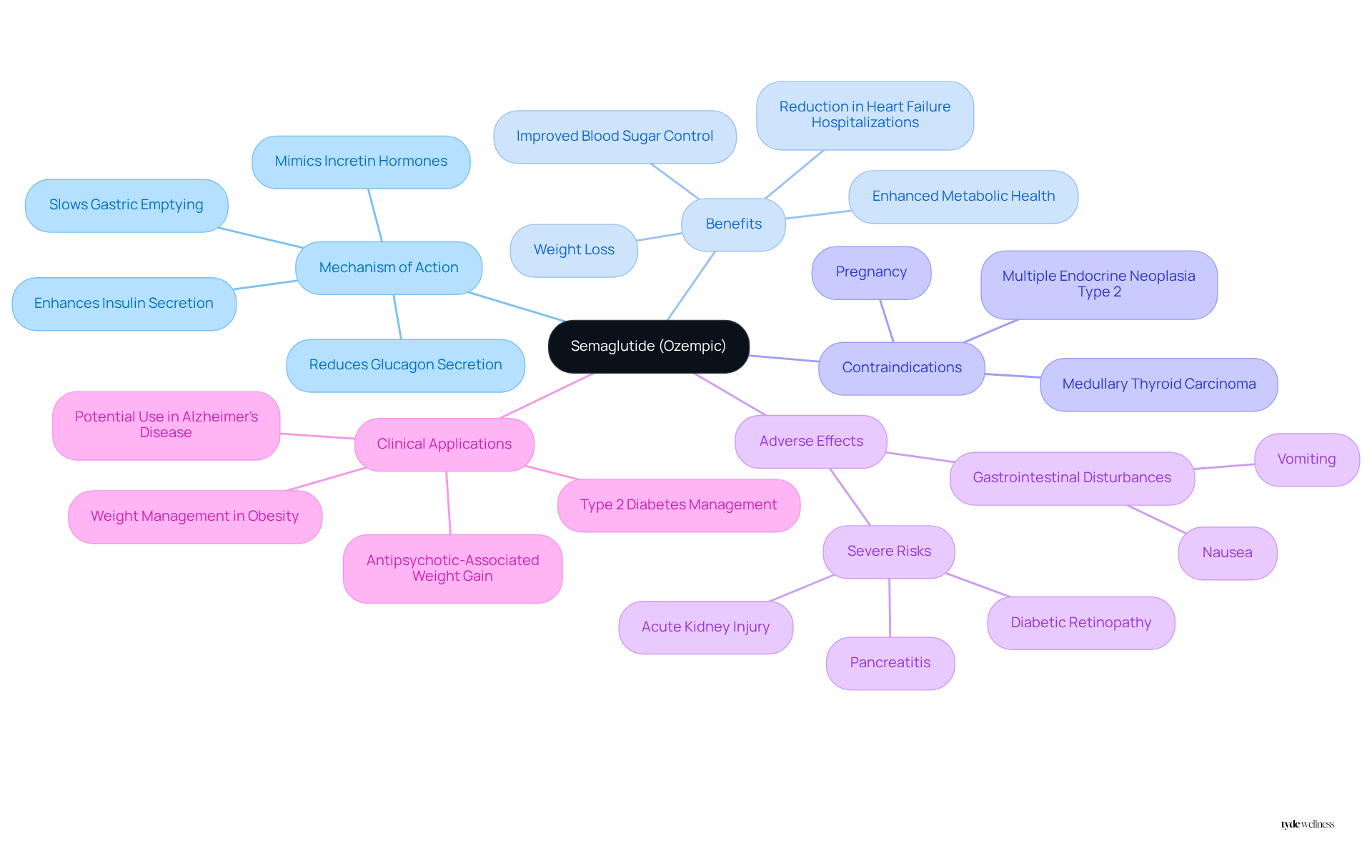
The medication known generically as semaglutide is a GLP-1 receptor agonist that plays a crucial role in managing Type 2 diabetes. By mimicking incretin hormones, which are naturally produced in response to food intake, semaglutide effectively lowers blood sugar levels. It achieves this by enhancing insulin secretion, reducing glucagon secretion, and slowing gastric emptying. This multifaceted approach not only aids in blood sugar control but also promotes weight loss, making it particularly beneficial for individuals facing due to hormonal fluctuations during perimenopause or menopause.
At Tyde Wellness, we utilize FDA-approved GLP-1 treatments such as semaglutide and tirzepatide, which are clinically demonstrated to aid in effective and sustainable weight loss. Our personalized doctor-prescribed GLP-1 medications ensure a tailored approach to weight loss that includes comprehensive support through nutrition plans and ongoing coaching. The effectiveness of this medication in real-world situations has been remarkable, with many users reporting significant weight loss and enhanced metabolic health, highlighting its value as a treatment choice for those going through these life transitions.
However, it is important to note that semaglutide therapy is contraindicated in individuals with medullary thyroid carcinoma and multiple endocrine neoplasia type 2, as well as in those who are pregnant due to potential adverse fetal outcomes. Common adverse effects include gastrointestinal disturbances like nausea and vomiting. Notably, semaglutide has also been associated with a 70% reduction in heart failure hospitalizations, highlighting its potential benefits beyond weight management. The medication was approved by the FDA in 2017 for treating Type 2 diabetes, further establishing its credibility as a treatment option.
Explore Blue Cross Blue Shield Coverage Criteria for Ozempic
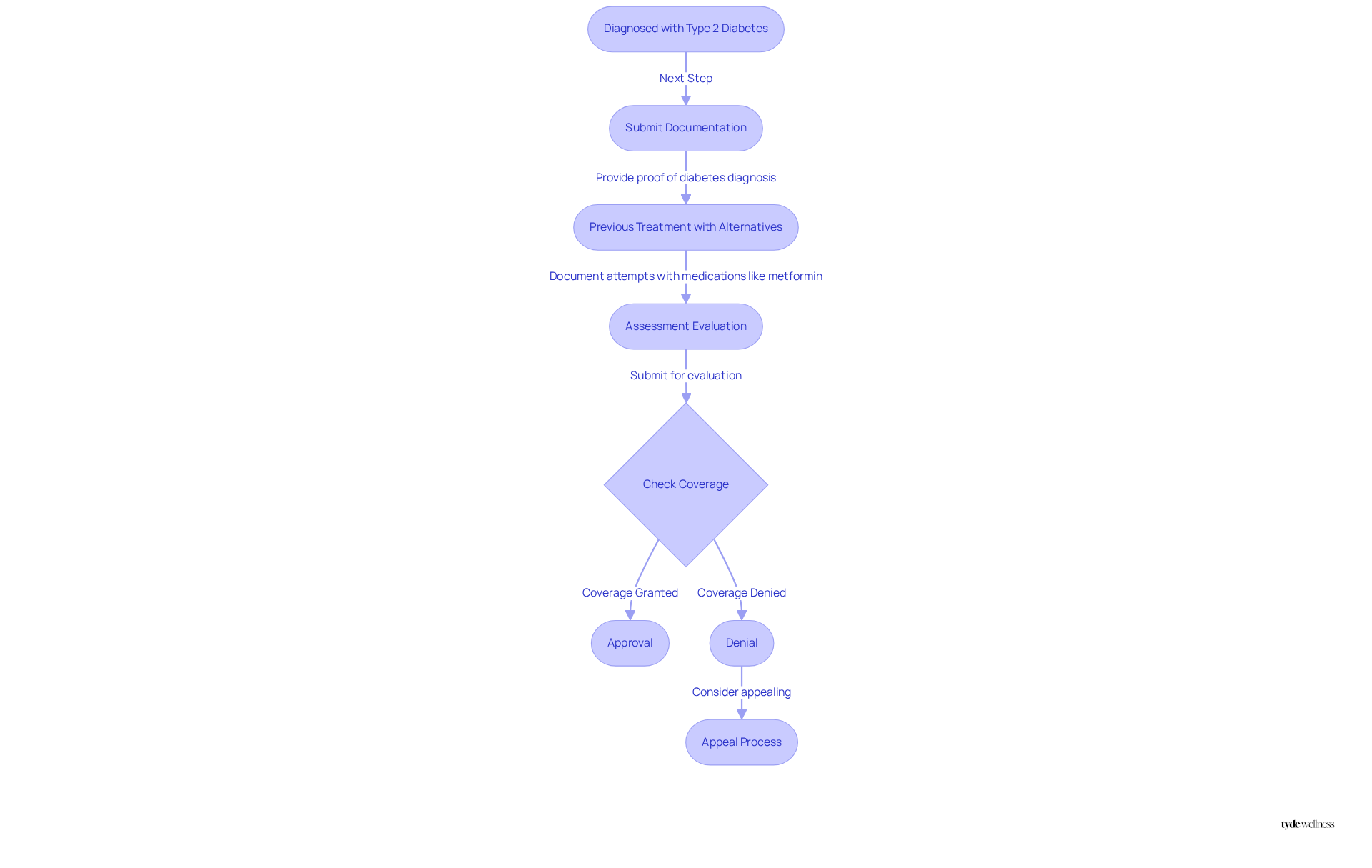
A common inquiry is whether Blue Cross covers Ozempic, as Blue Cross Blue Shield (BCBS) typically provides benefits for Ozempic when prescribed for individuals diagnosed with Type 2 diabetes. However, the question of whether Blue Cross covers Ozempic can vary significantly based on the specific insurance plan, the individual’s medical history, and the necessity for prior authorization. Typically, BCBS requires individuals to submit . Furthermore, individuals may need to demonstrate that they have previously attempted treatment with alternative medications, such as metformin, prior to the approval of this medication. This multi-step process is crucial for individuals to navigate effectively, as understanding these criteria can significantly enhance their chances of figuring out if Blue Cross covers Ozempic for this essential medication.
The cost of the medication without insurance can be substantial, ranging from approximately $800 to $900 for a month’s supply. However, individuals may qualify for an Ozempic Savings Card, allowing them to pay as little as $25 for a supply, thereby increasing accessibility.
Real-life examples illustrate the complexities of BCBS benefits for GLP-1 medications. Some patients have successfully secured insurance by meticulously documenting their medical history and demonstrating the ineffectiveness of prior treatments. Conversely, others have encountered denials because they were uncertain about whether Blue Cross covers Ozempic due to insufficient evidence of medical necessity or because it was not included in their plan’s formulary.
Experts emphasize the importance of being well-informed about the assessment evaluation process. Insurance specialists note that BCBS evaluates coverage requests, including whether Blue Cross covers Ozempic, based on established medical guidelines and the specific individual’s treatment history. Notably, BCBS will discontinue coverage of GLP-1 medications in large group fully insured plans starting January 1, 2025, which could impact many individuals. This underscores the necessity for individuals to prepare thorough documentation when seeking approval for the medication, ensuring they meet all specified criteria. Additionally, patients should consult a healthcare professional to ascertain their eligibility for the medication and verify if it is included in their plan’s formulary, as this directly influences the approval process and out-of-pocket costs.
Check Your Plan: Steps to Verify Ozempic Coverage with Blue Cross
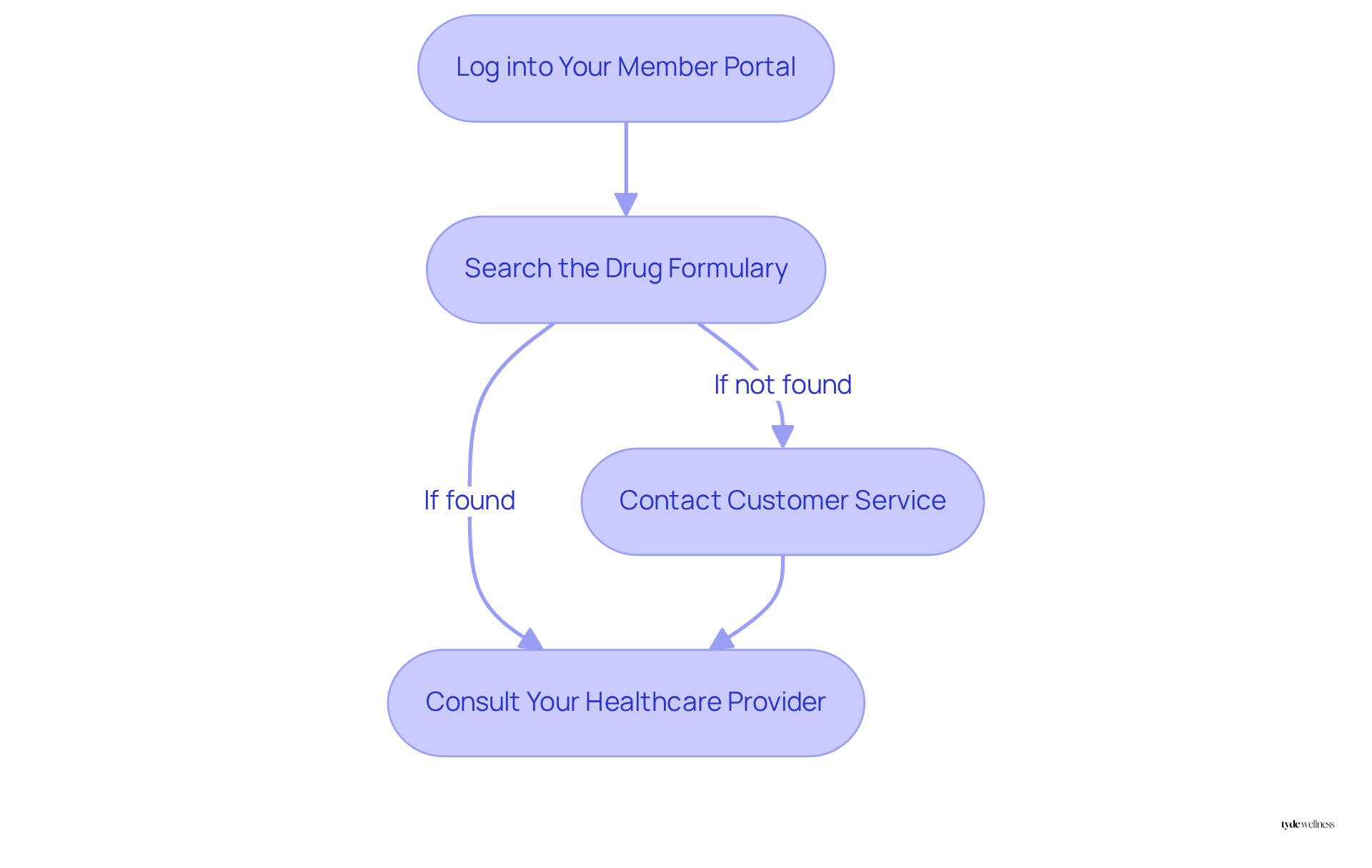
To determine if Ozempic is covered by your Blue Cross plan, follow these steps:
- Log into Your Member Portal: Begin by accessing your Blue Cross member account online. This portal typically contains your plan details, including covered medications.
- Search the Drug Formulary: Navigate to the formulary or drug list section. Search for ‘Ozempic’ to determine if it is included and to see if it does Blue Cross cover Ozempic, as this will influence your copay.
- Contact Customer Service: If the information is not available online, call the customer service number on your insurance card. Be prepared to provide your member ID and inquire about specific details related to the medication’s benefits.
- Consult Your Healthcare Provider: Discuss the necessity of Ozempic with your doctor. They can assist in supplying the documentation necessary for prior authorization, which is often needed for approval.
Understanding your is crucial, as it can significantly impact your out-of-pocket costs. A 2023 survey indicated that many Blue Cross members successfully confirm their medication benefits, underscoring the importance of these steps in navigating insurance complexities.
Troubleshoot Coverage Issues: What to Do If Ozempic Is Denied
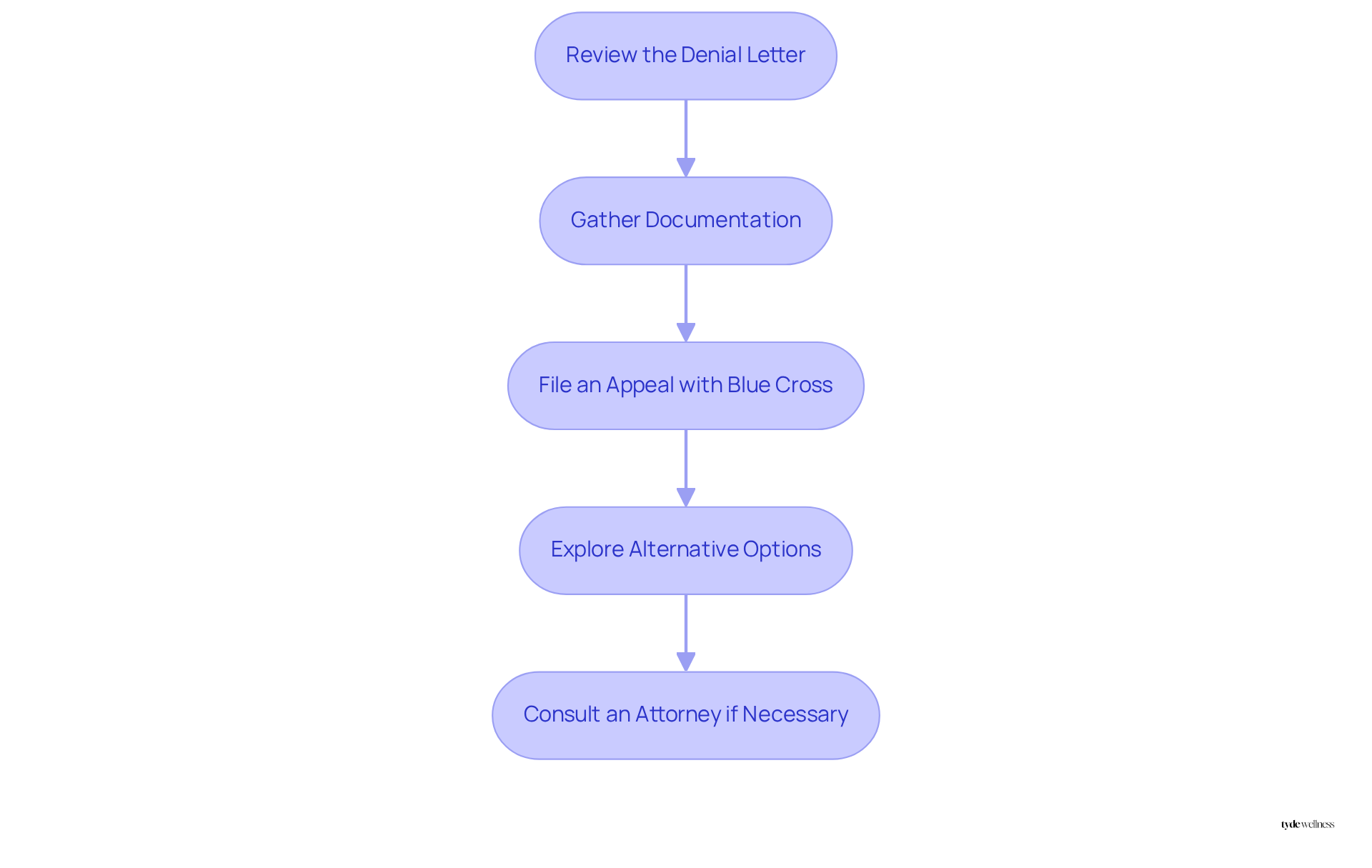
If your request for Ozempic coverage is denied, follow these steps to navigate the appeals process effectively:
- Review the Denial Letter: Carefully examine the denial letter to understand the specific reasons for the denial. Common issues include claims of lack of medical necessity or the drug not being included on the insurance formulary.
- Gather Documentation: Compile all relevant medical records and documentation from your healthcare provider that support the necessity for the medication. This may encompass treatment history, prior drugs attempted, and any supporting letters from your doctor.
- I need to find out does Blue Cross cover Ozempic. To find out if Blue Cross covers Ozempic, file an appeal by reaching out to them to initiate the appeal process. Submit the required documentation along with a clear explanation of why you believe the denial should be overturned. Highlight any clinical benefits and health enhancements linked to the use of the medication, as these factors can strengthen your case. Remember, the like Ozempic can exceed $1,000 without insurance coverage, making it essential to advocate for your needs.
- Explore Alternative Options: If your appeal is unsuccessful, consider inquiring about assistance programs or manufacturer discounts that could help reduce costs. Additionally, discuss with your healthcare provider the possibility of alternative medications that may be covered under your plan.
Navigating insurance challenges can be daunting; however, understanding your rights and options is crucial. Many patients have successfully appealed denials by providing comprehensive documentation and advocating for their health needs. As Dr. Kimberly Gudzune noted, engaging with healthcare advocates can provide valuable insights into overcoming these obstacles. If you continue to face challenges, consulting with a qualified attorney experienced in insurance denials can help clarify your rights and options.
Conclusion
Understanding the intricacies of insurance coverage for medications like Ozempic is vital for those managing Type 2 diabetes and seeking effective treatment options. This guide outlines essential steps and considerations for determining whether Blue Cross Blue Shield covers Ozempic, emphasizing the importance of thorough documentation and understanding individual plan specifics.
Key insights include the multifaceted benefits of Ozempic, which not only aids in blood sugar management but also promotes weight loss and reduces hospitalizations related to heart failure. The article elaborates on the coverage criteria established by Blue Cross, highlighting the necessity for prior authorization and documentation of medical necessity. Furthermore, it provides practical steps for verifying coverage, troubleshooting potential denials, and advocating for necessary treatments.
In navigating the complexities of insurance coverage, individuals are encouraged to remain proactive and informed. Engaging with healthcare providers, understanding insurance policies, and being prepared to appeal denials can significantly influence access to essential medications like Ozempic. The journey to effective diabetes management should not be hindered by insurance barriers; taking these steps can empower individuals to secure the treatment they need for a healthier future.
Frequently Asked Questions
What is Ozempic and how does it work?
Ozempic, generically known as semaglutide, is a GLP-1 receptor agonist used to manage Type 2 diabetes. It mimics incretin hormones to lower blood sugar levels by enhancing insulin secretion, reducing glucagon secretion, and slowing gastric emptying.
What are the benefits of semaglutide for weight management?
Semaglutide not only aids in blood sugar control but also promotes weight loss, making it beneficial for individuals facing weight management challenges, especially during hormonal fluctuations in perimenopause or menopause.
How is semaglutide prescribed at Tyde Wellness?
At Tyde Wellness, semaglutide is prescribed as part of FDA-approved GLP-1 treatments tailored to individual needs. This includes comprehensive support through nutrition plans and ongoing coaching to ensure effective and sustainable weight loss.
What results have users reported from using semaglutide?
Many users have reported significant weight loss and enhanced metabolic health, demonstrating the medication’s effectiveness in real-world situations, particularly for those undergoing life transitions.
Who should avoid using semaglutide?
Semaglutide therapy is contraindicated for individuals with medullary thyroid carcinoma, multiple endocrine neoplasia type 2, and those who are pregnant due to potential adverse fetal outcomes.
What are the common side effects of semaglutide?
Common adverse effects of semaglutide include gastrointestinal disturbances such as nausea and vomiting.
What additional health benefits does semaglutide provide?
Semaglutide has been associated with a 70% reduction in heart failure hospitalizations, indicating its potential benefits beyond weight management.
When was semaglutide approved by the FDA?
Semaglutide was approved by the FDA in 2017 for treating Type 2 diabetes, establishing its credibility as a treatment option.
List of Sources
- Understand Ozempic: What It Is and How It Works
- How does Ozempic work? Understanding GLP-1s for diabetes, weight loss, and beyond – Harvard Health (https://health.harvard.edu/staying-healthy/how-does-ozempic-work-understanding-glp-1s-for-diabetes-weight-loss-and-beyond)
- Naturally occurring molecule rivals Ozempic in weight loss, sidesteps side effects (https://med.stanford.edu/news/all-news/2025/03/ozempic-rival.html)
- How Does Ozempic Work? (Published 2024) (https://nytimes.com/2024/05/20/well/live/ozempic-weight-loss-drugs.html)
- Weight Loss Drug Shows Benefits for Heart Failure – News Center (https://news.feinberg.northwestern.edu/2024/05/08/weight-loss-drug-shows-benefits-for-heart-failure)
- Semaglutide: Double-edged Sword with Risks and Benefits – PMC (https://pmc.ncbi.nlm.nih.gov/articles/PMC11790292)
- Explore Blue Cross Blue Shield Coverage Criteria for Ozempic
- Blue Cross Blue Shield of Michigan pulling back on GLP-1 coverage (https://fiercehealthcare.com/payers/blue-cross-blue-shield-michigan-pulling-back-glp-1-coverage)
- Does Blue Cross Blue Shield Cover Ozempic (https://getcurex.com/drug-insurance/does-blue-cross-blue-shield-cover-ozempic?srsltid=AfmBOoqG_sIKtO6UdqPC9Ef1oCZdIXz37nThaYI2nIctgbD8KsYupspN)
- Is Ozempic Covered by Insurance? – GoodRx (https://goodrx.com/ozempic/is-ozempic-covered-by-insurance?srsltid=AfmBOopiy-6ecNefJ7nrBFUBUXBBxZl64a6LjcvMSsbzow6aZyp931_a)
- Does Medicare cover Ozempic? – WTOP News (https://wtop.com/health-fitness/2024/05/does-medicare-cover-ozempic)
- Check Your Plan: Steps to Verify Ozempic Coverage with Blue Cross
- Does Blue Cross Blue Shield Cover Ozempic? | Ro (https://ro.co/weight-loss/does-blue-cross-blue-shield-cover-ozempic)
- Does Blue Cross Blue Shield cover Ozempic? (https://nicerx.com/blog/does-blue-cross-blue-shield-cover-ozempic)
- Changes to insurance coverage for weight loss drugs are coming in 2025 (https://whyy.org/articles/independence-blue-cross-restrict-coverage-ozempic-weight-loss)
- Does Blue Cross Blue Shield cover Ozempic? (https://singlecare.com/blog/does-blue-cross-blue-shield-cover-ozempic)
- Troubleshoot Coverage Issues: What to Do If Ozempic Is Denied
- Insurance denials for popular new weight loss medications leave patients with risky choices | CNN (https://cnn.com/2024/01/08/health/weight-loss-drug-insurance-denials)
- Denial of Ozempic, Wegovy, Mounjaro, Zepbound Coverage (https://gmlawyers.com/denied-health-coverage-for-weight-loss-medications-how-to-fight-back)
- How to get insurance to cover Ozempic (https://getheally.com/patients/news/how-to-get-insurance-to-cover-ozempic)
- Alarmed by popularity of Ozempic and Wegovy, insurers wage multi-front battle (https://statnews.com/2023/08/03/ozempic-wegovy-obesity-weight-loss-drugs-insurers)