Overview
Kaiser Permanente’s coverage for weight loss drugs is primarily determined by specific medical necessity criteria. Typically, these medications are covered for obesity-related health conditions rather than for purely aesthetic reasons.
Starting January 1, 2025, Kaiser will implement an exclusion for certain weight loss medications unless they are prescribed for patients with a BMI over 40. This change underscores the importance of understanding individual plan details and eligibility requirements. By navigating these aspects effectively, patients can ensure they receive the appropriate coverage.
Introduction
Navigating the complexities of health insurance can be particularly daunting, especially concerning weight loss medications. As Kaiser Permanente prepares to revise its coverage criteria in 2025, many individuals are left uncertain about their access to essential treatments for obesity-related conditions. This article explores the details of Kaiser’s coverage for weight loss drugs, offering readers vital insights and practical steps to assess their eligibility. What challenges may emerge in securing coverage, and how can individuals effectively advocate for their health needs amid these changes?
Understand the Basics of Insurance Coverage for Weight Loss Drugs
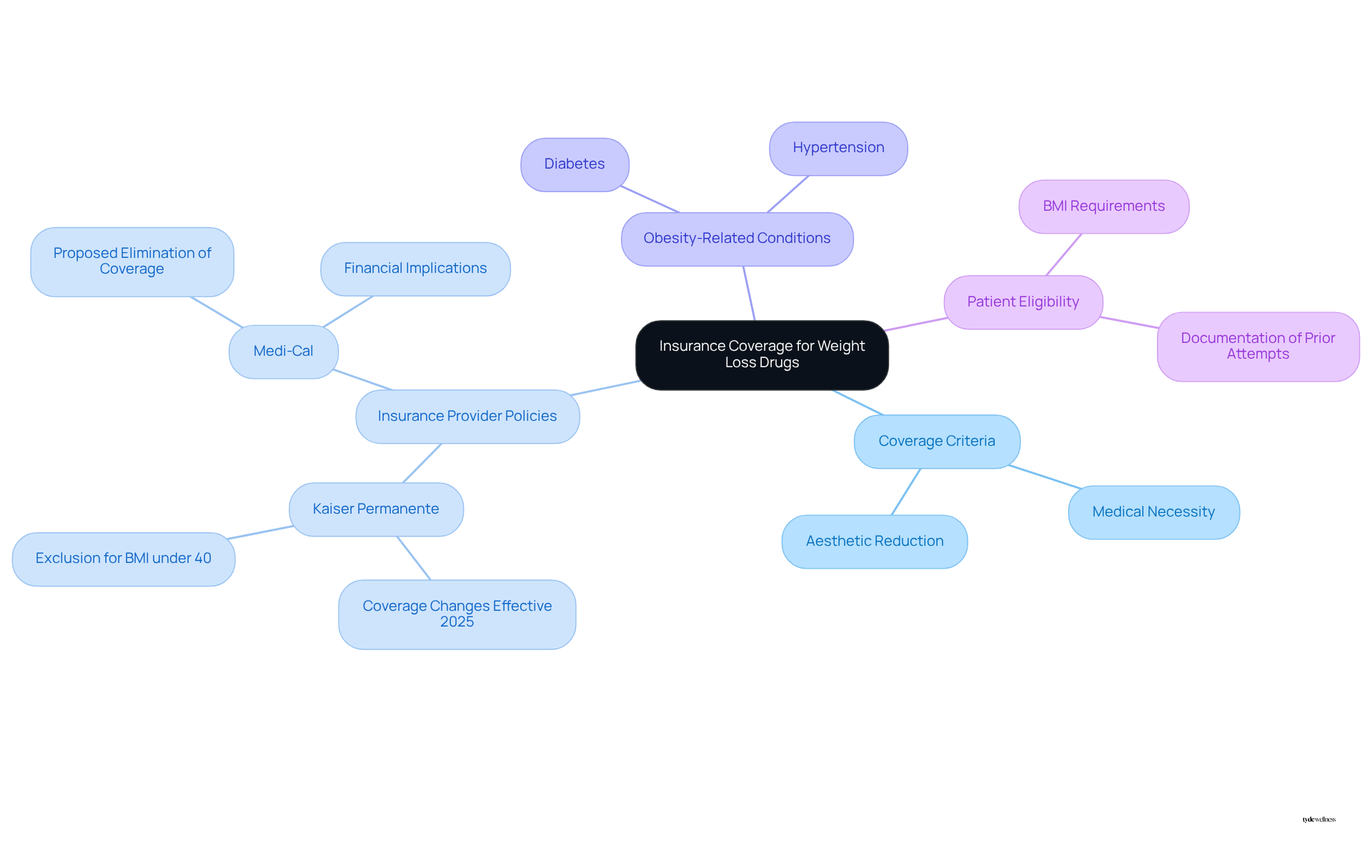
Insurance protection for slimming drugs varies significantly based on the specific plan and the medical necessity of the therapy. Most insurance providers, including Kaiser Permanente, generally cover treatments for obesity-related medical issues such as diabetes or hypertension when prescribed, but the question remains: does Kaiser cover weight loss drugs? However, if the treatment is prescribed solely for aesthetic reduction, reimbursement may be denied.
For instance, Kaiser Permanente plans to revise its coverage criteria starting January 1, 2025, leading to inquiries about whether Kaiser covers weight loss drugs, as it will exclude coverage for GLP-1 medications when prescribed exclusively for reducing body mass in patients with a BMI under 40. This shift indicates a broader trend among insurers, where approximately 60% of plans include medications for obesity-related conditions, though stringent criteria often apply.
At Tyde Wellness, our program is designed for individuals seeking a personalized approach to weight loss and sustainable wellness. If you are overweight or obese (with a BMI of 25 or higher) or have one or more obesity-related conditions, you may be a suitable candidate for GLP-1 therapy. Our initial consultation will evaluate your health, goals, and lifestyle to determine the most effective plan for you.
To navigate these complexities, it is essential to familiarize yourself with the terms of your insurance policy, including any exclusions or requirements for prior authorization. Certain plans may require documentation of previous attempts to lose weight or evidence of obesity-related health concerns before approving support for GLP-1 therapy. Understanding these fundamentals will empower you to make informed decisions regarding your management options and ensure you receive the .
Check Your Kaiser Plan Details for Weight Loss Drug Coverage
To determine your Kaiser plan’s coverage for weight loss medications, follow these steps:
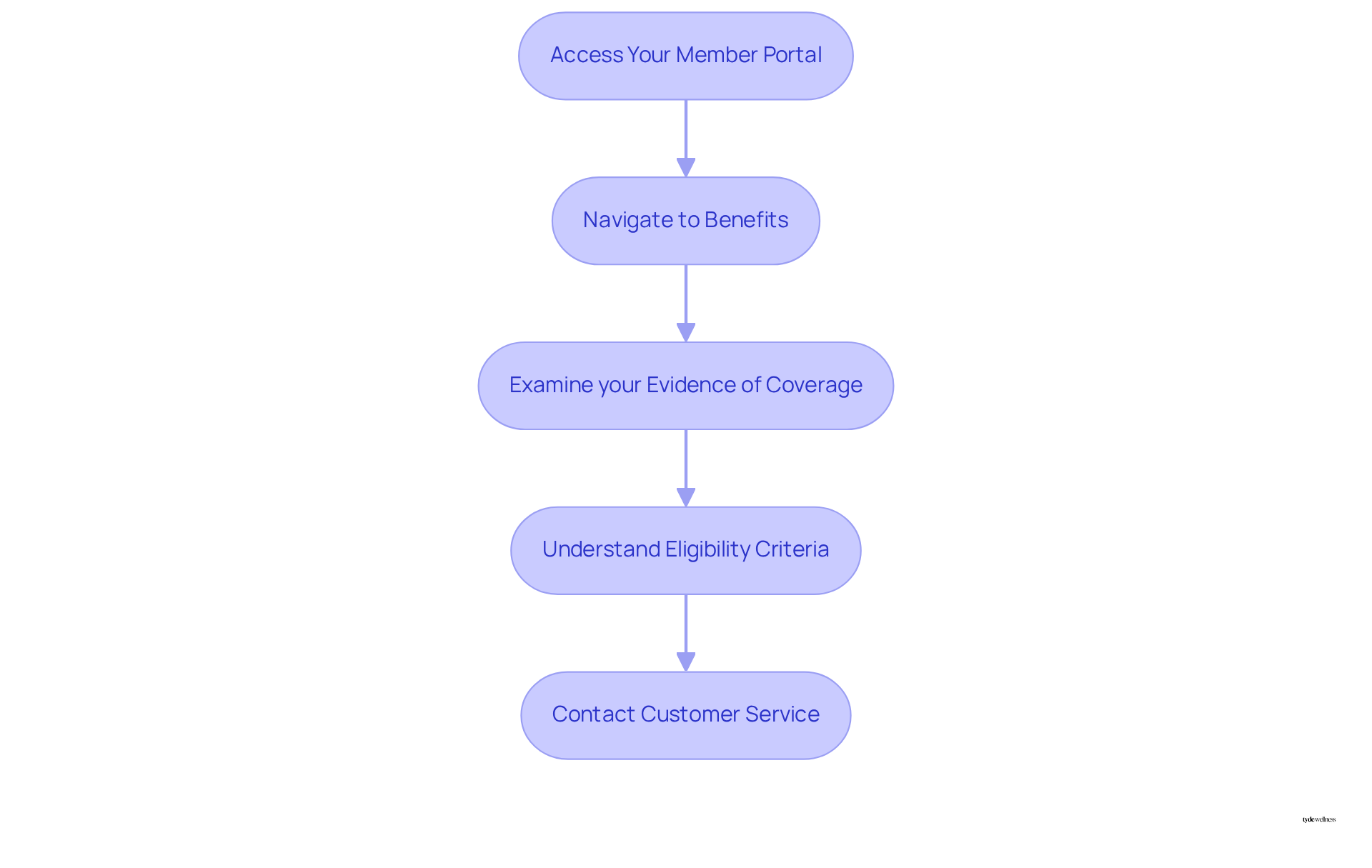
- Access Your Member Portal: Log in to your Kaiser Permanente member account via the website or mobile app.
- Navigate to Benefits: Locate the section labeled ‘Benefits’ or ‘Coverage Information.’
- Examine your Evidence of Coverage: This document outlines what is encompassed in your plan, including specific criteria for treatments related to reducing body mass, specifically addressing whether Kaiser covers weight loss drugs. Pay attention to any updates regarding policy changes effective January 1, 2025, which may influence your access to GLP-1 drugs.
- Understand Eligibility Criteria: Familiarize yourself with the criteria for to see if Kaiser covers weight loss drugs, as this will help you identify what information is necessary for your request.
- Contact Customer Service: If you have any questions or need further clarification, reach out to Kaiser’s customer service. They can offer detailed information about your insurance and assist you with the required steps for obtaining prescriptions. Be prepared for the possibility of contesting a denial, as persistence may be necessary to secure support.
Identify Common Barriers to Coverage and How to Overcome Them
Recognizing shared obstacles to accessing obesity medications is essential for navigating the healthcare environment. Key obstacles include:
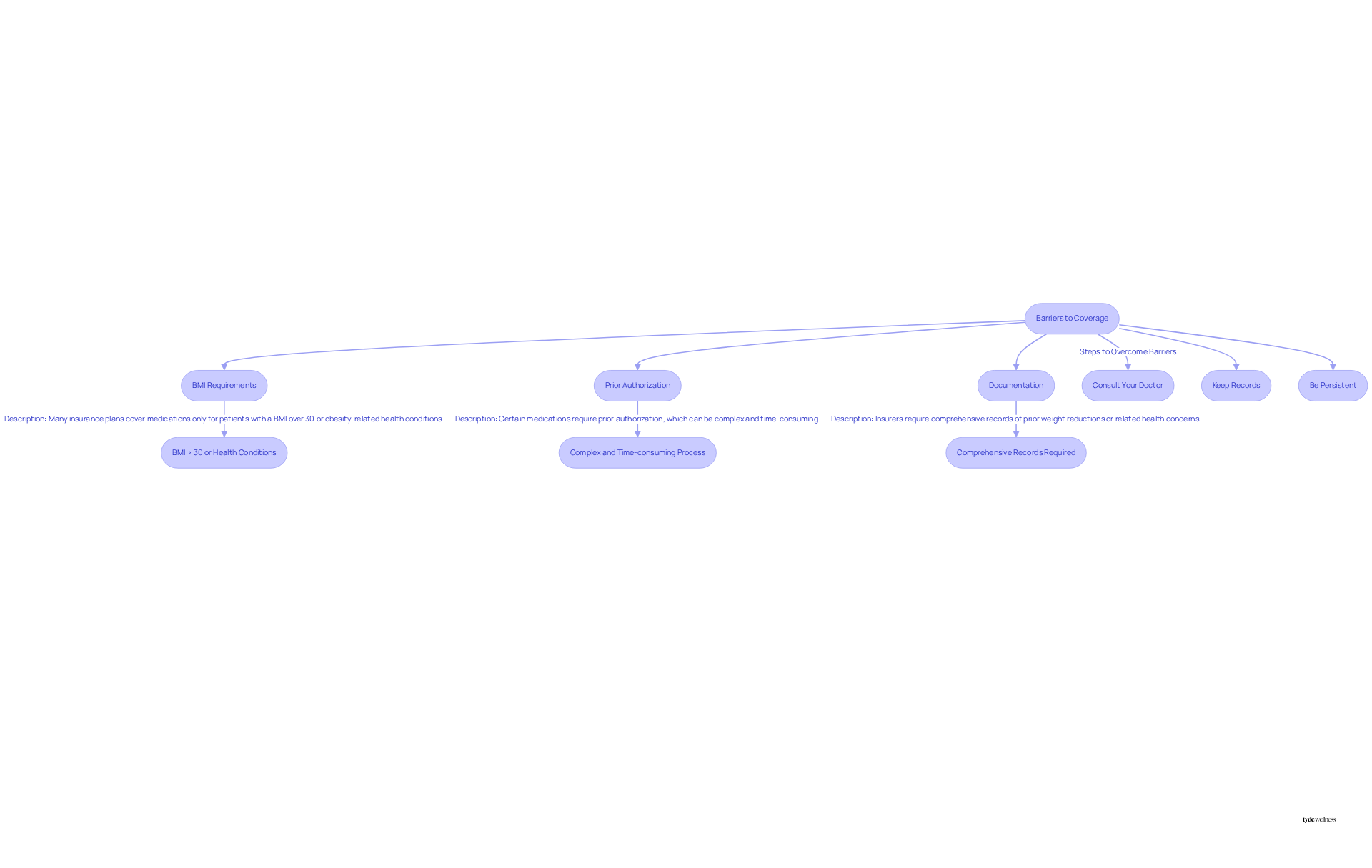
- BMI Requirements: Many insurance plans, including Kaiser Permanente, typically cover weight loss medications only for patients with a Body Mass Index (BMI) over 30 or those with obesity-related health conditions. Starting January 1, 2025, benefits for GLP-1 medications will be eliminated from base plans for patients with a BMI under 40 when prescribed solely for reducing body mass.
- Prior Authorization: Certain medications require prior authorization, meaning your healthcare provider must justify the prescription before approval is granted. This process can be complex and time-consuming.
- Documentation: Insurers frequently require comprehensive records of prior weight reductions or related health concerns, which can pose an obstacle for many patients.
To overcome these barriers:
- Consult Your Doctor: Ensure your healthcare provider understands your insurance requirements and can provide the necessary documentation to support your case.
- Keep Records: Maintain a detailed account of your weight reduction journey and any related health issues to strengthen your request for insurance coverage.
- Be Persistent: If you encounter a denial, do not hesitate to appeal the decision and provide additional information as needed. This proactive approach can significantly enhance your chances of securing the required coverage.
Learn How to Appeal a Denied Coverage Request for Weight Loss Drugs
If your request for coverage of weight loss medications is denied, follow these steps to effectively appeal the decision:
-
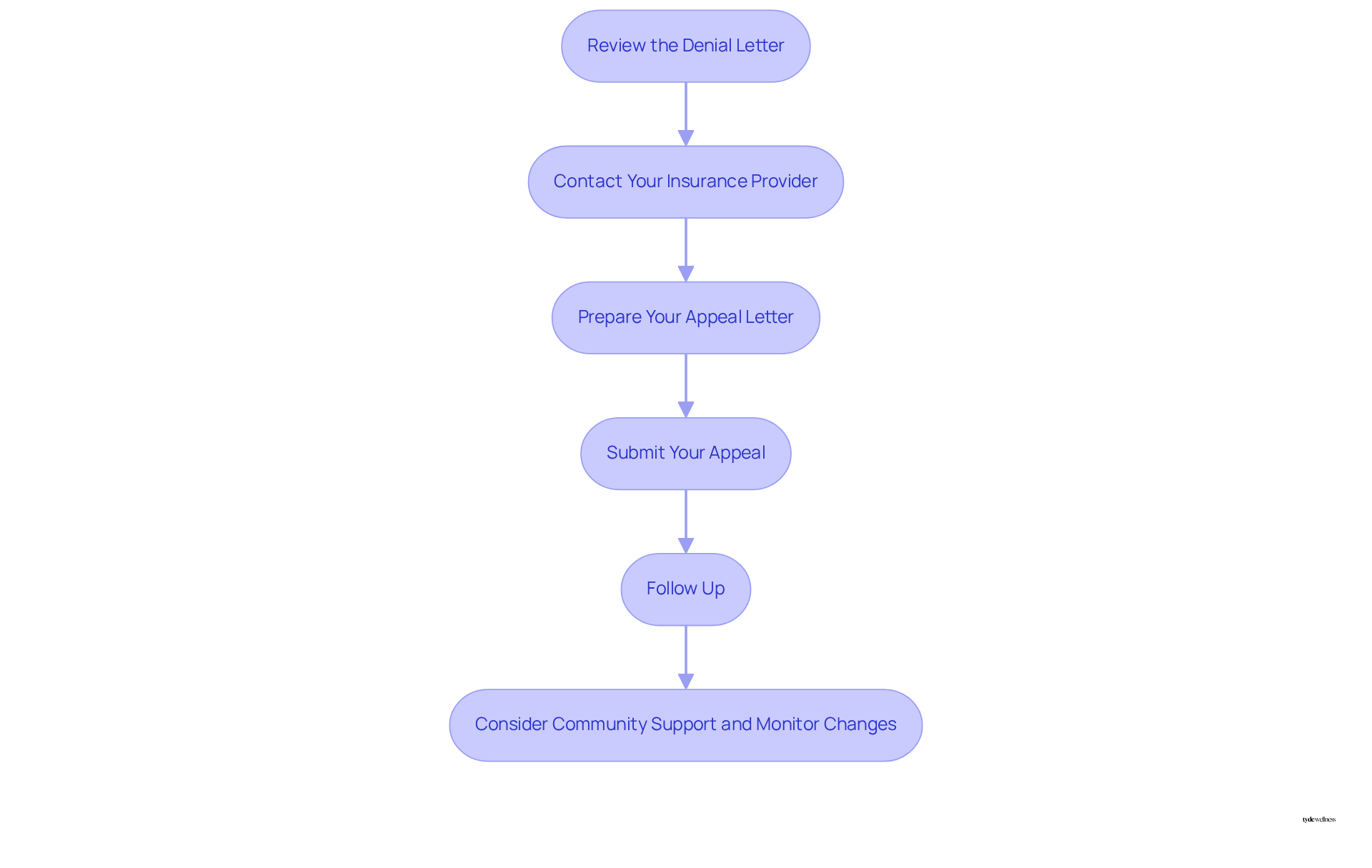
Review the Denial Letter: Carefully examine the letter to understand the specific reasons for the denial. This will help you gather the necessary documentation for your appeal.
-
Contact Your Insurance Provider: Reach out to Kaiser’s customer service to discuss the denial. Clarify any questions you have about the appeals process and gather additional information that may assist your case, especially if it relates to whether Kaiser covers weight loss drugs.
-
Prepare Your Appeal Letter: Draft a clear and concise appeal letter that includes:
- Your personal information and policy number.
- A thorough explanation outlining why you think the treatment should be covered, citing any pertinent health conditions.
- Supporting documents, such as medical records or letters from your healthcare provider, that demonstrate the necessity of the treatment.
-
Submit Your Appeal: Send your appeal letter and all supporting documentation to the address specified in the denial letter. Be sure to keep copies of everything for your records.
-
Follow Up: After submitting your appeal, follow up with your insurance provider to check on the status of your request. Persistence can be key, as many successful appeals often result from consistent communication.
In California, the average success rate for appeals regarding whether can vary, but many patients have successfully overturned denials by providing comprehensive documentation and demonstrating the clinical benefits of the medications. As a Tyde Circle member, you can leverage community support by sharing experiences and gathering insights that may strengthen your appeal. Remember, timely action is crucial; if your insurance is denied, addressing the issue promptly can help secure the necessary treatments for your health. Additionally, be informed that changes may arise regarding whether Kaiser Permanente covers weight loss drugs, as they will modify benefits for GLP-1 medications starting January 1, 2025, which may affect your appeal. High out-of-pocket costs for medications like Zepbound or Wegovy can also pose significant financial burdens, making it essential to advocate for your coverage.
Conclusion
Understanding the nuances of insurance coverage for weight loss drugs is crucial for those seeking assistance in managing obesity and its related health conditions. This article highlights the importance of knowing your specific Kaiser Permanente plan details and the evolving criteria that could affect coverage, especially with upcoming changes set for January 1, 2025. By being informed about the conditions under which weight loss medications are covered, individuals can better navigate their healthcare options.
Key points discussed include:
- The necessity of medical documentation
- The impact of BMI requirements
- The potential for denial of coverage based solely on aesthetic reasons
Additionally, a roadmap for appealing denied claims is provided, emphasizing the importance of persistence and thorough documentation. By following these outlined steps, individuals can enhance their chances of securing the necessary support for their weight loss journey.
Ultimately, advocating for one’s health by understanding insurance policies and actively engaging with healthcare providers can lead to significant benefits. As the landscape of weight loss drug coverage continues to evolve, staying informed and proactive is essential. For those considering weight loss medications, taking the initiative to explore coverage options and prepare for potential obstacles can make a substantial difference in achieving health goals.
Frequently Asked Questions
What factors influence insurance coverage for weight loss drugs?
Insurance coverage for weight loss drugs varies based on the specific plan and the medical necessity of the therapy. Most providers cover treatments for obesity-related medical issues but may deny reimbursement for treatments prescribed solely for aesthetic purposes.
What changes are expected in Kaiser Permanente’s coverage for weight loss drugs?
Starting January 1, 2025, Kaiser Permanente plans to exclude coverage for GLP-1 medications when prescribed exclusively for reducing body mass in patients with a BMI under 40.
What percentage of insurance plans cover medications for obesity-related conditions?
Approximately 60% of insurance plans include medications for obesity-related conditions, although they often have stringent criteria for coverage.
Who is a suitable candidate for GLP-1 therapy at Tyde Wellness?
Individuals who are overweight or obese (with a BMI of 25 or higher) or have one or more obesity-related conditions may be suitable candidates for GLP-1 therapy.
What should individuals do to understand their insurance coverage for weight loss drugs?
It is essential to familiarize oneself with the terms of the insurance policy, including exclusions and requirements for prior authorization. Some plans may require documentation of previous weight loss attempts or evidence of obesity-related health concerns.
How can individuals navigate the complexities of insurance coverage for weight loss therapies?
Understanding the fundamentals of their insurance policy and seeking a thorough evaluation of their health, goals, and lifestyle can empower individuals to make informed decisions regarding their management options and ensure they receive necessary support.
List of Sources
- Understand the Basics of Insurance Coverage for Weight Loss Drugs
- Trump Won’t Force Medicaid To Cover GLP-1s for Obesity. A Few States Are Doing It Anyway. – KFF Health News (https://kffhealthnews.org/news/article/glp1-drugs-weight-loss-obesity-trump-medicaid-coverage-south-carolina)
- Medi-Cal coverage of weight loss drugs on chopping block under CA proposal (https://calmatters.org/health/2025/05/medi-cal-coverage-weight-loss-drugs-newsom-california)
- Kaiser Permanente Changes Coverage for Weight Loss Drugs (https://warnerpacific.com/education-and-events/news/2024/kaiser-permanente-changes-coverage-for-weight-loss-drugs)
- Check Your Kaiser Plan Details for Weight Loss Drug Coverage
- Medical Weight Management Program FAQs | Kaiser Permanente Medical Weight Management Program (https://kphealthyweight.com/faqs)
- How to find out if weight loss drugs are covered by your insurance, and what to do if they’re not (https://trib.com/news/nation-world/business/personal-finance/article_bdf7dc9d-dce6-5329-94ca-321588b476d2.html)
- Major insurance changes are coming for weight loss drugs. Here’s how it could affect patients (https://wisn.com/article/insurance-changes-glp-weight-loss-drugs/65264795)
- Kaiser Permanente Changes Coverage for Weight Loss Drugs (https://warnerpacific.com/education-and-events/news/2024/kaiser-permanente-changes-coverage-for-weight-loss-drugs)
- Identify Common Barriers to Coverage and How to Overcome Them
- Major insurance changes are coming for weight loss drugs. Here’s how it could affect patients (https://kcci.com/article/insurance-changes-glp-weight-loss-drugs/65264795)
- Changes GLP 1 AOM 2025 (https://business.kaiserpermanente.org/business/broker/california/news-and-announcements/2024/glp-1-coverage-changes-2025)
- Trump Won’t Force Medicaid To Cover GLP-1s for Obesity. A Few States Are Doing It Anyway. – KFF Health News (https://kffhealthnews.org/news/article/glp1-drugs-weight-loss-obesity-trump-medicaid-coverage-south-carolina)
- Many Insurers Do Not Cover Drugs Approved To Help People Lose Weight – KFF Health News (https://kffhealthnews.org/news/many-insurers-do-not-cover-drugs-approved-to-help-people-lose-weight)
- Learn How to Appeal a Denied Coverage Request for Weight Loss Drugs
- Insurance denials for popular new weight loss medications leave patients with risky choices | CNN (https://cnn.com/2024/01/08/health/weight-loss-drug-insurance-denials)
- Denial of Ozempic, Wegovy, Mounjaro, Zepbound Coverage (https://gmlawyers.com/denied-health-coverage-for-weight-loss-medications-how-to-fight-back)
- Kaiser Permanente Changes Coverage for Weight Loss Drugs (https://warnerpacific.com/education-and-events/news/2024/kaiser-permanente-changes-coverage-for-weight-loss-drugs)
- What to Do When Your Insurance Denies Zepbound or Wegovy – A Pound of Cure | A Bariatric Surgery and Non-Surgical Weight Loss practice in Tucson, AZ (https://poundofcureweightloss.com/insurance-denies-zepbound-or-wegovy)